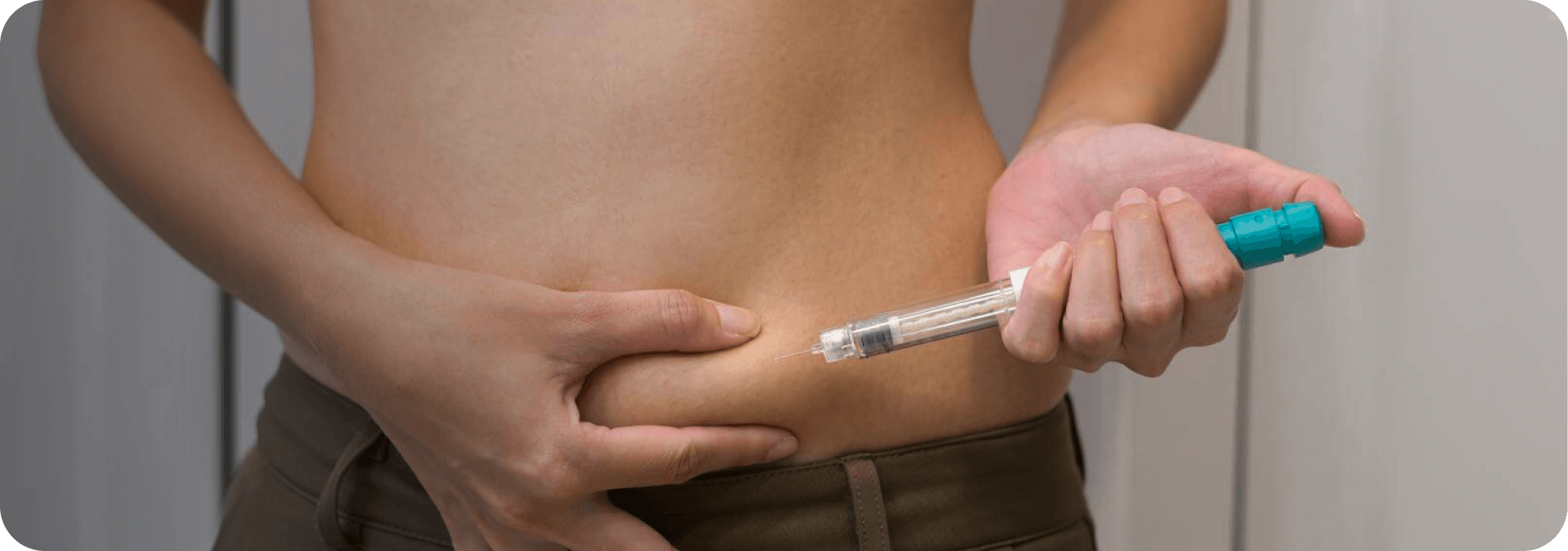
Ovulation induction is a fertility treatment designed to help women who have irregular periods or trouble ovulating. The goal is to stimulate the ovaries to produce eggs, increasing the chances of conception.

During ovulation induction, medications are used to encourage the ovaries to develop healthy follicles, which contain the eggs. To get started, your hormone levels and ovarian health will be assessed and based on these results, you may be prescribed either oral medications or hormone injections to stimulate egg production.
Throughout the treatment, regular check-ups, including blood tests and ultrasounds will help monitor your progress and determine the best time for conception.

Ovulation induction is suitable for women who have irregular periods or aren’t ovulating regularly. This includes conditions like polycystic ovary syndrome (PCOS), thyroid issues, and hormonal imbalances.
To see if ovulation induction is right for you, your overall health and medical history will be reviewed. Things like your age, hormone levels, and how your ovaries are functioning will be considered. It’s also important to talk about any other medical conditions you have and any medications you’re taking, as these can influence your options.
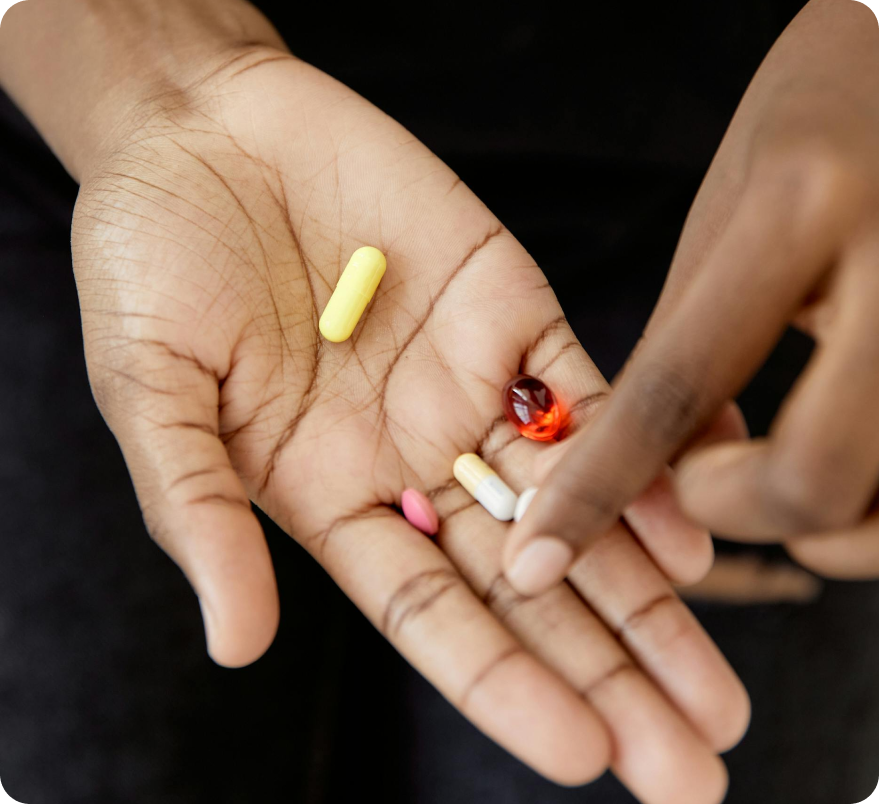
There are many reasons why ovulation may not be occurring, and the choice of medication for Ovulation Induction depends on the underlying cause. Treatments include oral medications (Letrozole or Clomiphene) and subcutaneous injections (FSH).
Oral medications like Letrozole and Clomiphene are typically taken for five days. These medications work in different ways to stimulate ovulation:
Letrozole reduces estrogen levels.
Clomiphene blocks estrogen receptors in the pituitary gland.
Both mechanisms prompt the pituitary gland to increase the release of FSH (follicle-stimulating hormone), encouraging the growth of a follicle in the ovary. These medications are commonly prescribed for women with PCOS, though in some cases, FSH injections may also be used.
FSH injections are often recommended when ovulation issues stem from inadequate signalling by the pituitary gland. A daily dose of FSH directly stimulates the growth of a follicle in the ovary.
Ovulation can occur naturally or may require a ‘trigger’ injection. The main challenge with FSH treatment is ensuring that only one follicle develops. Without careful monitoring through blood tests and ultrasounds, there is a risk of multiple pregnancies.
For this reason, we ask that couples abstain from unprotected intercourse until they are told it is safe.
Monitoring is an important part of ovulation induction to ensure the treatment’s safety and effectiveness. Regular check-ups allow us to track your progress and make adjustments as needed. These appointments may involve blood tests and ultrasounds:
This careful monitoring ensures that the treatment is working effectively and supports the best possible outcome for your fertility journey.

The process begins with a comprehensive consultation where I’ll review your medical history, assess your hormone levels, and evaluate your ovarian function. Based on these findings, I’ll develop a personalised treatment plan tailored to your needs.
You’ll start with prescribed medications, either oral or injectable, to stimulate egg development.
Throughout the cycle, you’ll have regular blood tests and ultrasounds to monitor follicle growth and hormone levels.
Once the follicles are ready, I’ll advise you on the best time for conception. This may involve natural intercourse or fertility procedures like intrauterine insemination (IUI).
After the treatment cycle, we’ll discuss the results and determine any necessary adjustments for future cycles if needed.
For further information on Ovulation Induction:

The journey to pregnancy is unique for everyone, and I’m here to support you every step of the way. My passion lies in providing hopeful parents with compassionate, evidence-based care.
By taking a holistic approach to fertility, I address a wide range of challenges and offer personalised pathways to help you achieve your dream of starting or growing your family. Together, we’ll make empowered, informed decisions that align with your goals and values.
Ovulation Induction (OI) refers to the use of medication to stimulate follicle growth and facilitate ovulation.
OI is largely performed for couples where the cause of infertility is ovulatory dysfunction.
Medications used may be oral (Letrozole or Clomiphene) or subcutaneous injections (FSH).
The medication used in OI will be determined by the underlying cause.
For instance, Letrozole or Clomiphene is most commonly used in women with PCOS. Whereas, FSH injections is most commonly used in women where the lack of ovulation is due to inadequate signalling from the pituitary gland. There will be occasions however, where FSH may be used for women with PCOS.
For further information on OI:
Daily dose FSH will directly stimulate a follicle in the ovary to grow.
Five days of oral Letrozole or Clomiphene will either reduce a woman’s estrogen level (Letrozole) or, block estrogen receptors in the pituitary gland (Clomiphene). Either way, the pituitary will respond to this drop (or perceived drop) in estrogen and respond by increasing FSH. The rise in FSH will stimulate a follicle in the ovary to grow.
Ovulation will either occur naturally or with the aid of a ‘trigger’ injection.
The second half of the cycle is often supported with progesterone.
The main concern with OI is the inability to achieve the development of only one follicle.
Without careful monitoring (via hormonal blood tests and ultrasound) there is a risk of multiple pregnancies.
For this reason, we ask that couples abstain from unprotected intercourse until they are told it is safe.
The aim is to achieve monthly chances of success based on female age.
The main concern with OI is the inability to achieve the development of only one follicle.
Without careful monitoring (via hormonal blood tests and ultrasound) there is a risk of multiple pregnancies.
For this reason, we ask that couples abstain from unprotected intercourse until they are told it is safe.
Dr Anthony Marren partners with Genea Fertility. Patient Relationship Coordinators (PRCs) will provide a quote based on the treatment plan plus Medicare/ insurance status.
For further information on costs of fertility treatment in Sydney: https://www.genea.com.au/treatment-costs.
Understanding the emotional journey couples endure when they have difficulty conceiving or recurrent pregnancy loss is essential to my approach.
Creative Advertising by Kiin Agency.